Protect Your Skeleton's Health
 Our bones functions are to protect organs, to provide structure/act as the body’s frame work, to anchor muscles, and to store calcium. The optimal bone building years are childhood and young adulthood. As children grow and mature, their bone mass increases until it reaches peak bone mass or PBM. About 90 percent of peak bone mass (PBM) is acquired by age 18 in girls and age 20 in boys, according to the National Osteoporosis Foundation.
Our bones functions are to protect organs, to provide structure/act as the body’s frame work, to anchor muscles, and to store calcium. The optimal bone building years are childhood and young adulthood. As children grow and mature, their bone mass increases until it reaches peak bone mass or PBM. About 90 percent of peak bone mass (PBM) is acquired by age 18 in girls and age 20 in boys, according to the National Osteoporosis Foundation.
Bones are constantly changing with new bone being formed and old bone being broken down. When one is young, your body makes new bone more quickly than it breaks down old bone which is called remodeling. After PBM is acquired, bone remodeling continues but most adults lose more bone mass than they gain. The higher one’s PBM, the more bone you have, resulting in a reduced risk of developing osteoporosis.
Decreasing bone density or bone loss is part of the aging process. Osteoporosis affects the spongy interior of bones known as trabecular bone, and the outer bone layer, called cortical bone. Osteoporosis or brittle bone disease is often not diagnosed until a bone is broken. Risk factors contributing to the development of osteoporosis include:
- Gender. Women are at greater risk than men of developing osteoporosis due to their smaller bone mass.
- Size: Those with small body frames or a body mass index of 19 or less since you may have less bone mass to draw from as you age.
- Family History & Race: Having a parent or sibling who has osteoporosis. Those who are white or of Asian descent.
- Hormone levels. Bone loss increases with high thyroid hormone levels. As we age, men experience declining testosterone levels and women experience lower estrogen levels, both of which contribute to bone loss.
- Health conditions. Those with anorexia or bulimia are at an increased risk for bone loss. Conditions which affect your body’s ability to absorb calcium increase the risk of bone loss. These include Crohn’s disease, celiac disease, Cushing’s disease, stomach and weight loss surgery.
- Medications. Bone health is at risk with long-term use of corticosteroid medications (prednisone, cortisone, prednisolone, and dexamethasone); aromatase inhibitors, some anti-seizure medications; proton pump inhibitors, and selective serotonin reuptake inhibitors. Discuss your bone health with your primary healthcare provider if prescribed any of these medications.
- Tobacco & Alcohol Use. Research suggests tobacco contributes to weakening bones. More than 2 alcoholic drinks a day decrease the body’s ability to absorb calcium increasing the chances of developing osteoporosis.
Youth is the optimal time to build strong bones but adults can also take steps to protect their bone health. Low-impact weight-bearing cardiovascular exercises that require you to stand and support your body weight aids in keeping bones strong and helps to decrease bone loss. Examples are fast walking outdoors, treadmill walking, low-impact aerobics, Tai chi, dancing, using a stair machine or elliptical. Muscle strengthening activities such as weight lifting, use of elastic exercise bands, yoga, Pilates, or weight machines helps build bones, strengthens muscles, and improves balance. Adapt fall prevention, strategies such as removing throw rugs, use night lights, use shower mats, install bathroom grab bars and raised toilet seats.
The most common cause of osteoporosis is having a genetic predisposition followed by inadequate nutrition. Choosing healthy foods can aid in preventing bone loss. Two of the most important nutrients for bone health are calcium and vitamin D. The Institute of Medicine (IOM) recommends adults consume 1000 to 1200 milligrams (mg) per day with the upper limit being 2500 mg/day. Good calcium food sources are fat-free yogurt, skim milk, soy milk, tofu enriched with calcium, edamame, white beans, bok choy, kale, collard greens, broccoli, and almonds.
Vitamin D is essential for the development and maintenance of bone and aids with calcium absorption. Vitamin D is made in our skin when exposed to ultraviolet B rays which could contribute to skin damage, premature aging, and skin cancer. Food sources and supplements as discussed with your physician are the best ways to obtain Vitamin D. The IOM recommends 800- 1000 IU for falls and fracture prevention.
The nutrient rock stars for bone health are calcium and Vitamin D. However, there are other nutrients that aid in building and supporting bone health. They and some of their food sources are listed in the table below:
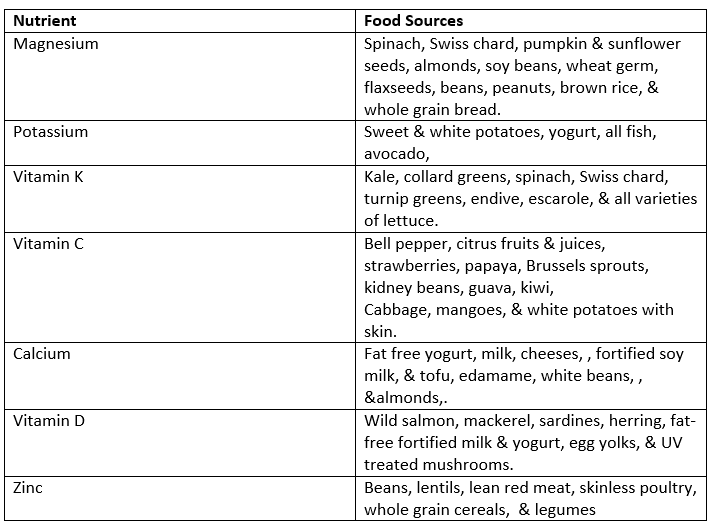
Research finds overweight and underweight individuals have a higher fracture risk. Staying at a healthy weight and engaging in regular physical activity helps to increase or at least aid in maintaining our bone density. According to the American Academy of Orthopedic Surgeons, preventing falls is vital to aid in preserving bones since half of all fractures are due to falls. A healthy eating plan, fall prevention strategies, physical activity, and maintaining a healthy weight are all important for the health of your skeleton.
Always consult with your physician or healthcare provider before making any dietary/nutrition changes or commencing or changing your physical activity.
